Abstract
Post-transplant diabetes mellitus occurs in 30–50% of cases during the first year post-renal transplantation. It is associated with increased morbidity, mortality and healthcare costs. Risk factors include age and specific immunosuppression regimens. At the same time, renal transplantation is increasingly indicated in elderly (aged >65 years) patients as this proportion of older patients in the prevalent dialysis population has increased. The immune system and β cells undergo senescence and this impacts on the risk for developing post-transplant diabetes and our ability to prevent such development. It may, however, be possible to identify patients at risk of developing post-transplant diabetes, enabling treatment protocols that prevent or reduce the impact of post-transplant diabetes. Much work remains to be completed in this area and is facilitated by the growing base of knowledge regarding the pathophysiology of post-transplant diabetes. Should post-transplant diabetes develop, there are a range of treatment options available. There is increasing interest in using newer agents, although their safety and efficacy in transplant recipients remains to be conclusively established.

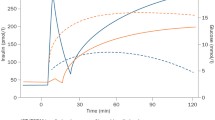
Reproduced with the permission of the authors [6]

Reproduced with the permission of the authors [6]
Similar content being viewed by others
References
Bergrem HA, Valderhaug TG, Hartmann A, et al. Undiagnosed diabetes in kidney transplant candidates: a case-finding strategy. Clin J Am Soc Nephrol. 2010;5(4):616–22.
Sharif A, Hecking M, de Vries AP, et al. Proceedings from an international consensus meeting on posttransplantation diabetes mellitus: recommendations and future directions. Am J Transplant. 2014;14(9):1992–2000.
Caillard S, Eprinchard L, Perrin P, et al. Incidence and risk factors of glucose metabolism disorders in kidney transplant recipients: role of systematic screening by oral glucose tolerance test. Transplantation. 2011;91(7):757–64.
Hornum M, Jorgensen KA, Hansen JM, et al. New-onset diabetes mellitus after kidney transplantation in Denmark. Clin J Am Soc Nephrol. 2010;5(4):709–16.
Iida S, Ishida H, Tokumoto T, et al. New-onset diabetes after transplantation in tacrolimus-treated, living kidney transplantation: long-term impact and utility of the pre-transplant OGTT. Int Urol Nephrol. 2010;42(4):935–45.
Langsford D, Obeyesekere V, Vogrin S, et al. A prospective study of renal transplant recipients: a fall in insulin secretion underpins dysglycemia after renal transplantation. Transplant Direct. 2016;2(11):e107.
ANZDATA Registry. 39th report, Australia and New Zealand Dialysis and Transplant Registry, Adelaide, Australia. 2017. Available from: http://www.anzdata.org.au. Accessed 30 June 2017.
UK Renal Registry. 18th annual report of the Renal Association. Nephron. 2016;132(Suppl. 1):69–98.
United States Renal Data System. 2016 USRDS annual data report: epidemiology of kidney disease in the United States. National Institutes of Health, 2016. Available from: http://www.usrds.org/adr.aspx. Accessed 30 June 2017.
Organ Procurement and Transplantation Network (OPTN) and Scientific Registry of Transplant Recipients (SRTR). OPTN/SRTR 2015 annual data report. Available from: http://www.srtr.org/reports-tools/srtroptn-annual-data-report/. Accessed 30 June 2017.
Stevens KK, Woo YM, Clancy M, et al. Deceased donor transplantation in the elderly: are we creating false hope? Nephrol Dial Transplant. 2011;26(7):2382–6.
Heldal K, Hartmann A, Grootendorst DC, et al. Benefit of kidney transplantation beyond 70 years of age. Nephrol Dial Transplant. 2010;25(5):1680–7.
Schold J, Srinivas TR, Sehgal AR, Meier-Kriesche HU. Half of kidney transplant candidates who are older than 60 years now placed on the waiting list will die before receiving a deceased-donor transplant. Clin J Am Soc Nephrol. 2009;4(7):1239–45.
Rao PS, Merion RM, Ashby VB, et al. Renal transplantation in elderly patients older than 70 years of age: results from the Scientific Registry of Transplant Recipients. Transplantation. 2007;83(8):1069–74.
Wolfe RA, Ashby VB, Milford EL, et al. Comparison of mortality in all patients on dialysis, patients on dialysis awaiting transplantation, and recipients of a first cadaveric transplant. N Engl J Med. 1999;341(23):1725–30.
Oniscu GC, Brown H, Forsythe JL. Impact of cadaveric renal transplantation on survival in patients listed for transplantation. J Am Soc Nephrol. 2005;16(6):1859–65.
McDonald SP, Russ GR. Survival of recipients of cadaveric kidney transplants compared with those receiving dialysis treatment in Australia and New Zealand, 1991–2001. Nephrol Dial Transplant. 2002;17(12):2212–9.
Tonelli M, Wiebe N, Knoll G, et al. Systematic review: kidney transplantation compared with dialysis in clinically relevant outcomes. Am J Transplant. 2011;11(10):2093–109.
Gill JS, Schaeffner E, Chadban S, et al. Quantification of the early risk of death in elderly kidney transplant recipients. Am J Transplant. 2013;13(2):427–32.
Vincenti F, Friman S, Scheuermann E, et al. Results of an international, randomized trial comparing glucose metabolism disorders and outcome with cyclosporine versus tacrolimus. Am J Transplant. 2007;7(6):1506–14.
Prasad N, Gurjer D, Bhadauria D, et al. Is basiliximab induction, a novel risk factor for new onset diabetes after transplantation for living donor renal allograft recipients? Nephrology. 2014;19(4):244–50.
Valderhaug TG, Hjelmesaeth J, Hartmann A, et al. The association of early post-transplant glucose levels with long-term mortality. Diabetologia. 2011;54(6):1341–9.
Hjelmesaeth J, Hartmann A, Leivestad T, et al. The impact of early-diagnosed new-onset post-transplantation diabetes mellitus on survival and major cardiac events. Kidney Int. 2006;69(3):588–95.
Cosio FG, Kudva Y, van der Velde M, et al. New onset hyperglycemia and diabetes are associated with increased cardiovascular risk after kidney transplantation. Kidney Int. 2005;67(6):2415–21.
Valderhaug TG, Hjelmesaeth J, Jenssen T, Roislien J, Leivestad T, Hartmann A. Early posttransplantation hyperglycemia in kidney transplant recipients is associated with overall long-term graft losses. Transplantation. 2012;94(7):714–20.
Heldal K, Hartmann A, Leivestad T, Foss A, Midtvedt K. Risk variables associated with the outcome of kidney recipients >70 years of age in the new millennium. Nephrol Dial Transplant. 2011;26(8):2706–11.
Shivaswamy V, Boerner B, Larsen J. Post-transplant diabetes mellitus: causes, treatment, and impact on outcomes. Endocr Rev. 2016;37(1):37–61.
Yates CJ, Fourlanos S, Colman PG, Cohney SJ. Screening for new-onset diabetes after kidney transplantation: limitations of fasting glucose and advantages of afternoon glucose and glycated hemoglobin. Transplantation. 2013;96(8):726–31.
Shabir S, Jham S, Harper L, et al. Validity of glycated haemoglobin to diagnose new onset diabetes after transplantation. Transpl Int. 2013;26(3):315–21.
Eide IA, Halden TA, Hartmann A, et al. Limitations of hemoglobin A1c for the diagnosis of posttransplant diabetes mellitus. Transplantation. 2015;99(3):629–35.
Cole EH, Johnston O, Rose CL, Gill JS. Impact of acute rejection and new-onset diabetes on long-term transplant graft and patient survival. Clin J Am Soc Nephrol. 2008;3(3):814–21.
Luan FL, Steffick DE, Ojo AO. New-onset diabetes mellitus in kidney transplant recipients discharged on steroid-free immunosuppression. Transplantation. 2011;91(3):334–41.
Silva HT, Yang HC, Meier-Kriesche HU, et al. Long-term follow-up of a phase III clinical trial comparing tacrolimus extended-release/MMF, tacrolimus/MMF, and cyclosporine/MMF in de novo kidney transplant recipients. Transplantation. 2014;97(6):636–41.
Pascual J, Royuela A, Galeano C, et al. Very early steroid withdrawal or complete avoidance for kidney transplant recipients: a systematic review. Nephrol Dial Transplant. 2012;27(2):825–32.
Woodle ES, First MR, Pirsch J, et al. Astellas Corticosteroid Withdrawal Study Group. A prospective, randomized, double-blind, placebo-controlled multicenter trial comparing early (7 day) corticosteroid cessation versus long-term, low-dose corticosteroid therapy. Ann Surg. 2008;248(4):564–77.
Lopez-Soler RI, Chan R, Martinolich J, et al. Early steroid withdrawal results in improved patient and graft survival and lower risk of post-transplant cardiovascular risk profiles: a single-center 10-year experience. Clin Transplant. 2017;31(2). doi:10.1111/ctr.12878 (epub 2017 Jan 24).
Pirsch JD, Henning AK, First MR, et al. New-onset diabetes after transplantation: results from a double-blind early corticosteroid withdrawal trial. Am J Transplant. 2015;15(7):1982–90.
Johnston O, Rose CL, Webster AC, Gill JS. Sirolimus is associated with new-onset diabetes in kidney transplant recipients. J Am Soc Nephrol. 2008;19(7):1411–8.
Masson P, Henderson L, Chapman JR, et al. Belatacept for kidney transplant recipients. Cochrane Database Syst Rev. 2014;(11):CD010699.
Montero N, Pascual J. Immunosuppression and post-transplant hyperglycemia. Curr Diabetes Rev. 2015;11(3):144–54.
Heit JJ, Apelqvist AA, Gu X, et al. Calcineurin/NFAT signalling regulates pancreatic beta-cell growth and function. Nature. 2006;443(7109):345–9.
Nagaraja P, Ravindran V, Morris-Stiff G, Baboolal K. Role of insulin resistance indices in predicting new-onset diabetes after kidney transplantation. Transpl Int. 2013;26(3):273–80.
Hecking M, Werzowa J, Haidinger M, et al. Novel views on new-onset diabetes after transplantation: development, prevention and treatment. Nephrol Dial Transplant. 2013;28(3):550–66.
Nam JH, Mun JI, Kim SI, et al. Beta-cell dysfunction rather than insulin resistance is the main contributing factor for the development of postrenal transplantation diabetes mellitus. Transplantation. 2001;71(10):1417–23.
Ohn JH, Kwak SH, Cho YM, et al. 10-year trajectory of β-cell function and insulin sensitivity in the development of type 2 diabetes: a community-based prospective cohort study. Lancet Diabetes Endocrinol. 2016;4(1):27–34.
Defronzo RA, Tripathy D, Schwenke DC, et al. Prediction of diabetes based on baseline metabolic characteristics in individuals at high risk. Diabetes Care. 2013;36(11):3607–12.
Bergman RN, Ader M, Huecking K, Van Citters G. Accurate assessment of beta-cell function: the hyperbolic correction. Diabetes. 2002;51(Suppl. 1):S212–20.
Helman A, Avrahami D, Klochendler A, et al. Effects of ageing and senescence on pancreatic β-cell function. Diabetes Obes Metab. 2016;18(Suppl. 1):58–62.
Suarez O, Pardo M, Gonzalez S, et al. Diabetes mellitus and renal transplantation in adults: is there enough evidence for diagnosis, treatment, and prevention of new-onset diabetes after renal transplantation? Transplant Proc. 2014;46(9):3015–20.
Madziarska K, Weyde W, Krajewska M, et al. The increased risk of post-transplant diabetes mellitus in peritoneal dialysis-treated kidney allograft recipients. Nephrol Dial Transplant. 2011;26(4):1396–401.
Chakkera HA, Weil EJ, Swanson CM, et al. Pretransplant risk score for new-onset diabetes after kidney transplantation. Diabetes Care. 2011;34(10):2141–5.
Tokodai K, Amada N, Haga I, Takayama T, Nakamura A. The 5-time point oral glucose tolerance test as a predictor of new-onset diabetes after kidney transplantation. Diabetes Res Clin Pract. 2014;103(2):298–303.
Heldal K, Midtvedt K. Managing transplant rejection in the elderly: the benefits of less aggressive immunosuppressive regimens. Drugs Aging. 2013;30(7):459–66.
Krenzien F, ElKhal A, Quante M, et al. A rationale for age-adapted immunosuppression in organ transplantation. Transplantation. 2015;99(11):2258–68.
McKay D, Jameson J. Kidney transplantation and the ageing immune system. Nat Rev Nephrol. 2012;8(12):700–8.
Fulop T, Larbi A, Witkowski JM, Kotb R, Hirokawa K, Pawelec G. Immunosenescence and cancer. Crit Rev Oncog. 2013;18(6):489–513.
Weinberger B, Grubeck-Loebenstein B. Vaccines for the elderly. Clin Microbiol Infect. 2012;18(Suppl. 5):100–8.
Noeldeke J, Fabrizii V, Arbogast H, et al. Prospective age-matching in elderly kidney transplant recipients: a 5-year analysis of the Eurotransplant Senior Program. Transplantation. 2006;82(1):141.
Tullius SG, Milford E. Kidney allocation and the aging immune response. N Engl J Med. 2011;364(14):1369–70.
Heldal K, Hartmann A, Leivestad T, et al. Clinical outcomes in elderly kidney transplant recipients are related to acute rejection episodes rather than pretransplant comorbidity. Transplantation. 2009;87(7):1045–51.
Hecking M, Haidinger M, Doller D, et al. Early basal insulin therapy decreases new-onset diabetes after renal transplantation. J Am Soc Nephrol. 2012;23(4):739–49.
Hermayer KL, Egidi MF, Finch NJ, et al. A randomized controlled trial to evaluate the effect of glycemic control on renal transplantation outcomes. J Clin Endocrinol Metab. 2012;97(12):4399–406.
Wallia A, Schmidt K, Oakes DJ, et al. Glycemic control reduces infections in post-liver transplant patients: results of a prospective, randomized study. J Clin Endocrinol Metab. 2017;102(2):451–9.
Aloi JA, Mulla C, Ullal J, Lieb DC. Improvement in inpatient glycemic care: pathways to quality. Curr Diab Rep. 2015;15(4):18.
Lipska KJ, Krumholz H, Soones T, Lee SJ. Polypharmacy in the aging patient: a review of glycemic control in older adults with type 2 diabetes. JAMA. 2016;315(10):1034–45.
LaFranca JA, Ijermans JNM, Betjes MGH, Dor FJMF. Body mass index and outcome in renal transplant recipients: a systematic review and meta-analysis. BMC Med. 2015;13:111.
von During ME, Jenssen T, Bollerslev J, et al. Visceral fat is better related to impaired glucose metabolism than body mass index after kidney transplantation. Transpl Int. 2015;28(10):1162–71.
Shah T, Kasravi A, Huang E, et al. Risk factors for development of new-onset diabetes mellitus after kidney transplantation. Transplantation. 2006;82(12):1673–6.
von During ME, Jenssen T, Bollerslev J, Asberg A, Godang K, Hartmann A. Visceral fat is strongly associated with post-transplant diabetes mellitus and glucose metabolism 1 year after kidney transplantation. Clin Transplant. 2017;31(1). doi:10.1111/ctr.12869 (epub 2016 Dec 15).
Ryan KJ, Casas JM, Mash LE, et al. The effect of intensive nutrition interventions on weight gain after kidney transplantation: protocol of a randomised controlled trial. BMC Nephrol. 2014;15:148.
Collins M, Plank L, Ryan K, et al. The INTENT trial: the effect of intensive nutrition interventions on weight gain after kidney transplantation: a randomized controlled trial. Perth: Asian Pacific Society of Nephrology; 2016.
Painter PL, Hector L, Ray K, et al. A randomized trial of exercise training after renal transplantation. Transplantation. 2002;74(1):42–8.
Didsbury M, McGee RG, Tong A, et al. Exercise training in solid organ transplant recipients: a systematic review and meta-analysis. Transplantation. 2013;95(5):679–87.
Lo C, Jun M, Badve SV, et al. Glucose-lowering agents for treating pre-existing and new-onset diabetes in kidney transplant recipients. Cochrane Database Syst Rev. 2017;(2):CD009966.
Kurian B, Joshi R, Helmuth A. Effectiveness and long-term safety of thiazolidinediones and metformin in renal transplant recipients. Endocr Pract. 2008;14(8):979–84.
Sharif A. Should metformin be our antiglycemic agent of choice post-transplantation? Am J Transplant. 2011;11(7):1376–81.
Hung AM, Roumie CL, Greevy RA, et al. Kidney function decline in metformin versus sulfonylurea initiators: assessment of time-dependent contribution of weight, blood pressure, and glycemic control. Pharmacoepidemiol Drug Saf. 2013;22(6):623–31.
Currie CJ, Poole CD, Gale EA. The influence of glucose-lowering therapies on cancer risk in type 2 diabetes. Diabetologia. 2009;52(9):1766–77.
Lalau JD, Arnouts P, Sharif A, De Broe ME. Metformin and other antidiabetic agents in renal failure patients. Kidney Int. 2015;87(2):308–22.
Stephen J, Anderson-Haag TL, Gustafson S, et al. Metformin use in kidney transplant recipients in the United States: an observational study. Am J Nephrol. 2014;40(6):546–53.
Tuerk TR, Bandur S, Nuernberger J, et al. Gliquidone therapy of new-onset diabetes mellitus after kidney transplantation. Clin Nephrol. 2008;70(1):26–32.
Dormandy JA, Charbonnel B, Eckland DJ, et al. Secondary prevention of macrovascular events in patients with type 2 diabetes in the PROactive Study (PROspective pioglitAzone Clinical Trial In macroVascular Events): a randomised controlled trial. Lancet. 2005;366(9493):1279–89.
Schneider CA, Ferrannini E, Defronzo R, Schernthaner G, Yates J, Erdmann E. Effect of pioglitazone on cardiovascular outcome in diabetes and chronic kidney disease. J Am Soc Nephrol. 2008;19(1):182–7.
Saemann MD, Krebs M. Thiazolidinediones in the treatment of patients with Post-Transplant-Hyperglycemia or new-onset diabetes mellitus after renal transplantation (NODAT): a new therapeutic option? Wien Klin Wochenschr. 2010;122(7–8):198–202.
Kim JW, Yang JH, Park HS, et al. Rosiglitazone protects the pancreatic beta-cell death induced by cyclosporine A. Biochem Biophys Res Commun. 2009;390(3):763–8.
Voytovich MH, Simonsen C, Jenssen T, Hjelmesaeth J, Asberg A, Hartmann A. Short-term treatment with rosiglitazone improves glucose tolerance, insulin sensitivity and endothelial function in renal transplant recipients. Nephrol Dial Transplant. 2005;20(2):413–8.
Halden TA, Egeland EJ, Asberg A, et al. GLP-1 restores altered insulin and glucagon secretion in posttransplantation diabetes. Diabetes Care. 2016;39(4):617–24.
Boerner BP, Miles CD, Shivaswamy V. Efficacy and safety of sitagliptin for the treatment of new-onset diabetes after renal transplantation. Int J Endocrinol. 2014;2014:617638.
Lane JT, Odegaard DE, Haire CE, Collier DS, Wrenshall LE, Stevens RB. Sitagliptin therapy in kidney transplant recipients with new-onset diabetes after transplantation. Transplantation. 2011;92(10):e56–7.
Haidinger M, Werzowa J, Hecking M, et al. Efficacy and safety of vildagliptin in new-onset diabetes after kidney transplantation: a randomized, double-blind, placebo-controlled trial. Am J Transplant. 2014;14(1):115–23.
Sanyal D, Gupta S, Das P. A retrospective study evaluating efficacy and safety of linagliptin in treatment of NODAT (in renal transplant recipients) in a real world setting. Indian J Endocrinol Metab. 2013;17(Suppl. 1):S203–5.
Zinman B, Wanner C, Lachin JM, et al. Empagliflozin, cardiovascular outcomes, and mortality in type 2 diabetes. N Engl J Med. 2015;373(22):2117–28.
Cherney D, Lund SS, Perkins BA, et al. The effect of sodium glucose cotransporter 2 inhibition with empagliflozin on microalbuminuria and macroalbuminuria in patients with type 2 diabetes. Diabetologia. 2016;59(9):1860–70.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
No sources of funding were received for the preparation of this article.
Conflict of interest
David Langsford, Adam Steinberg and Karen Dwyer have no conflicts of interest directly relevant to the content of this article.
Rights and permissions
About this article
Cite this article
Langsford, D., Steinberg, A. & Dwyer, K.M. Diabetes Mellitus Following Renal Transplantation: Clinical and Pharmacological Considerations for the Elderly Patient. Drugs Aging 34, 589–601 (2017). https://doi.org/10.1007/s40266-017-0478-2
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40266-017-0478-2