Abstract
Background
The Beck Depression Inventory (BDI) has been frequently employed as a measure of depression in studies of obesity, with the majority of studies reporting an improvement in scores following weight loss. Given the potential similarity in obesity-related and depressive symptoms, it is uncertain whether all components of depression would improve equally with weight loss.
Method
The study included obese patients who had undergone laparoscopic adjustable gastric banding (LAGB) surgery and had completed BDIs at baseline and 1 year after surgery. Two groups of patients were included, a general background group (N = 191, mean age = 41 ± 9, mean BMI = 43 ± 8) and a group identified as experiencing elevated depressive symptoms based on BDI scores ≥23 (EDS group; (N = 67, mean age = 40 ± 9, mean BMI = 45 ± 7).
Results
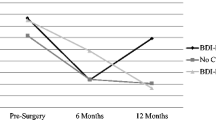
Overall, BDI scores fell for both groups, background group at baseline 17 ± 9–8 ± 7 at 1 year and for the EDS group at baseline 30 ± 5–14 ± 10 at 1 year. Patient scores on the negative self-attitude subscale were significantly greater than the two other subscales and showed the greatest improvement 1 year following LAGB. Preexisting antidepressant therapy had little or no association on the BDI scores or on its change following weight loss.
Conclusion
High rates of depression are continually reported in obesity, as is a remarkable decrease in depressive symptoms following weight loss. Negative attitudes towards one’s self appears to be driving elevated BDI scores rather than the overlap in physical symptoms between obesity and depression.
Similar content being viewed by others
References
WHO. Obesity: preventing and managing the global epidemic. Report of a WHO consultation. World Health Organ Tech Rep Ser. 2000;894:1–253.
Carpenter KM, Hasin DS, Allison DB, et al. Relationships between obesity and DSM-IV major depressive disorder, suicide ideation, and suicide attempts: results from a general population study. Am J Public Health. 2000;90(2):251–7.
Gertler R, Ramsey-Stewart G. Pre-operative psychiatric assessment of patients presenting for gastric bariatric surgery (surgical control of morbid obesity). Aust N Z J Surg. 1986;56(2):157–61.
Glinski J, Wetzler S, Goodman E. The psychology of gastric bypass surgery. Obes Surg. 2001;11:581–8.
Heo M, Pietrobelli A, Fontaine KR, et al. Depressive mood and obesity in US adults: comparison and moderation by sex, age, and race. Int J Obes (Lond). 2006;30(3):513–9.
Onyike CU, Crum RM, Lee HB, et al. Is obesity associated with major depression? Results from the Third National Health and Nutrition Examination Survey. Am J Epidemiol. 2003;158(12):1139–47.
Simon GE, Von Korff M, Saunders K, et al. Association between obesity and psychiatric disorders in the US adult population. Arch Gen Psychiatry. 2006;63(7):824–30.
Halmi KA, Long M, Stunkard AJ, et al. Psychiatric diagnosis of morbidly obese gastric bypass patients. Am J Psychiatry. 1980;137(4):470–2.
Werrij MQ, Mulkens S, Hospers HJ, Jansen A. Overweight and obesity: the significance of a depressed mood. Patient Educ Couns. 2006;62:126–31.
Larsen F. Psychosocial function before and after gastric banding surgery for morbid obesity. A prospective psychiatric study. Acta Psychiatr Scand Suppl. 1990;359:1–57.
Powers PS, Rosemurgy A, Boyd F, et al. Outcome of gasric restriction procedures: weight, psychiatric diagnoses, and satisfaction. Obes Surg. 1997;7:471–7.
Sarwer DB, Cohn NI, Gibbons LM, et al. Psychiatric diagnoses and psychiatric treatment among bariatric surgery candidates. Obes Surg. 2004;14:1148–56.
Guisado Macias JA, Vaz Leal FJ. Personality assessment in morbid obesity. German Journal of Psychiatry. 2002;5(4):90–4.
Black DW, Goldstein RB, Mason EE, et al. Depression and other mental disorders in the relatives of morbidly obese patients. J Affect Disord. 1992;25(2):91–5.
Hsu LK, Mulliken B, McDonagh B, et al. Binge eating disorder in extreme obesity. Int J Obes Relat Metab Disord. 2002;26(10):1398–403.
Dixon JB, Dixon ME, O'Brien PE. Depression in association with severe obesity: changes with weight loss. Arch Intern Med. 2003;163(17):2058–65.
Nickel C, Widermann C, Harms D, et al. Patients with extreme obesity: change in mental symptoms three years after gastric banding. Int J Psychiatry Med. 2005;35(2):109–22.
Sbrocco T, Nedegaard RC, Stone JM, et al. Behavioral choice treatment promotes continuing weight loss: preliminary results of a cognitive-behavioral decision-based treatment for obesity. J Consult Clin Psychol. 1999;67(2):260–6.
Venditti EM, Wing RR, Jakicic JM, et al. Weight cycling, psychological health, and binge eating in obese women. J Consult Clin Psychol. 1996;64(2):400–5.
Crisp AH, Queenan M, Sittampaln Y, et al. ‘Jolly fat’ revisited. J Psychosom Res. 1980;24(5):233–41.
Palinkas LA, Wingard DL, Barrett-Connor E. Depressive symptoms in overweight and obese older adults: a test of the “jolly fat” hypothesis. J Psychosom Res. 1996;40(1):59–66.
Olszanecka-Glinianowicz M, Zahorskamarkiewicz B, Kocelak P, et al. Depression in obese persons before starting complex group weight-reduction programme. Int J Soc Psychiatry. 2009;55(5):407–13.
de Wit LM, van Straten A, van Herten M, et al. Depression and body mass index, a u-shaped association. BMC Public Health. 2009;9:14.
Zhao G, Ford ES, Dhingra S, et al. Depression and anxiety among US adults: associations with body mass index. Int J Obes (Lond). 2009;33(2):257–66.
Delin CR, Watts JM, Bassett DL. An exploration of the outcomes of gastric bypass surgery for morbid obesity: patient characteristics and indeces of success. Obes Surg. 1995;5(2):159–70.
Dymek MP, le Grange D, Neven K, et al. Quality of life and psychosocial adjustment in patients after Roux-en-Y gastric bypass: a brief report. Obes Surg. 2001;11(1):32–9.
Ryden O, Hedenbro JL, Frederiksen SG. Weight loss after vertical banded gastroplasty can be predicted: a prospective psychological study. Obes Surg. 1996;6:237–43.
Waters GS, Pories WJ, Swanson MS, et al. Long-term studies of mental health after the Greenville gastric bypass operation for morbid obesity. Am J Surg. 1991;161(1):154–7. discussion 7–8.
Alger SA, Malone M, Cerulli J, et al. Beneficial effects of pharmacotherapy on weight loss, depressive symptoms, and eating patterns in obese binge eaters and non-binge eaters. Obes Res. 1999;7(5):469–76.
Brownell KD, Stunkard AJ. Couples training, pharmacotherapy, and behavior therapy in the treatment of obesity. Arch Gen Psychiatry. 1981;38(11):1224–9.
Chaput JP, Drapeau V, Hetherington M, et al. Psychobiological impact of a progressive weight loss program in obese men. Physiol Behav. 2005;86(1–2):224–32.
Fossati M, Amati F, Painot D, et al. Cognitive–behavioral therapy with simultaneous nutritional and physical activity education in obese patients with binge eating disorder. Eat Weight Disord. 2004;9(2):134–8.
Painot D, Jotterand S, Kammer A, et al. Simultaneous nutritional cognitive–behavioural therapy in obese patients. Patient Educ Couns. 2001;42(1):47–52.
Wadden TA, Stunkard AJ, Liebschutz J. Three-year follow-up of the treatment of obesity by very low calorie diet, behavior therapy, and their combination. J Consult Clin Psychol. 1988;56(6):925–8.
Wadden TA, Vogt RA, Andersen RE, et al. Exercise in the treatment of obesity: effects of four interventions on body composition, resting energy expenditure, appetite, and mood. J Consult Clin Psychol. 1997;65(2):269–77.
Faulconbridge LF, Wadden TA, Berkowitz RI, et al. Changes in symptoms of depression with weight loss: results of a randomized trial. Obesity (Silver Spring). 2009;17(5):1009–16.
Beck AT, Rush AJ, Shaw BF, et al. Cognitive therapy of depression. New York: Guilford; 1979.
Munoz DJ, Chen E, Fischer S, et al. Considerations for the use of the Beck Depression Inventory in the assessment of weight-loss surgery seeking patients. Obes Surg. 2007;17(8):1097–101.
Hayden MJ, Dixon JB, Dixon ME, et al. Confirmatory factor analysis of the Beck Depression Inventory in obese individuals seeking surgery. Obes Surg. 2010;20(4):432–9.
Krukowski RA, Friedman KE, Applegate KL. The utility of the Beck Depression Inventory in a bariatric surgery population. Obes Surg. 2010;20:426–31.
Plumb MM, Holland J. Comparative studies of psychological function in patients with advanced cancer—I. Self-reported depressive symptoms. Psychosom Med. 1977;39(4):264–76.
Clark DC, von Ammon Cavanaugh S, Gibbons RD. The core symptoms of depression in medical and psychiatric patients. J of Nerv Ment Dis. 1983;171(12):705–13.
Steer RA, Iguchi MY, Platt JJ. Use of the revised Beck Depression Inventory with intravenous drug users not in treatment. Psychol Addict Behav. 1992;6(4):225–32.
Beck AT, Beamesderfer A. Assessment of depression: the depression inventory. Mod Probl Pharmacopsychiatr. 1974;7:151–69.
Lasa L, Ayuso-Mateos JL, Vazquez-Barquero JL, et al. The use of the Beck Depression Inventory to screen for depression in the general population: a preliminary analysis. J Affect Disord. 2000;57(1–3):261–5.
Martisen EW, Friis S, Hoffart A. Assessment of depression: comparison between Beck Depression Inventory and subscales of Comprehensive Psychopathological Rating Scale. Acta Psychiatr Scand. 1995;92:460–3.
Sullivan MJ, Weinshenker B, Mikail S, et al. Screening for major depression in the early stages of multiple sclerosis. Can J Neurol Sci. 1995;22:228–31.
Geisser ME, Roth RS, Robinson ME. Assessing depression among persons with chronic pain using the Centre for Epidemiological Studies–Depression Scale and the Beck Depression Inventory: a comparative analysis. Clin J Pain. 1997;13:163–70.
Lustman PJ, Clouse RE, Griffith LS, et al. Screening for depression in diabetes using the Beck Depression Inventory. Psychosom Med. 1997;59:24–31.
Schotte CKW, Maes M, Cluydts R, et al. Construct validity of the Beck Depression Inventory in a depressive population. J Affect Disord. 1997;46:115–25.
Leetjens AF, Verhey FR, Luijckx GJ, et al. The validity of the Beck Inventory as a screening and diagnostic instrument for depression in patients with Parkinson's disease. Mov Disord. 2000;15:1221–4.
American Psychiatric Association. Diagnostic and statistical manual of mental disorders. 4th ed. Washington: American Psychiatric Association; 1994.
Kalarchian MA, Wilson GT, Brolin RE, et al. Binge eating in bariatric surgery patients. Int J Eat Disord. 1998;23(1):89–92.
Hayden MJ, Dixon JB, Dixon ME, O’Brien PE. Confirmatory factor analysis of the Beck Depression Inventory in obese individuals seeking surgery. Obes Surg. 2010;20:432–9.
Love RJ, Love AS, Bower S, et al. Impact of antidepressant use on gastric bypass surgery patients’ weight loss and health-related quality-of-life outcomes. Psychosomatics. 2008;49(6):478–86.
Acknowledgements
CORE receives unrestricted research funding from Allergan.
Disclosure
The authors declare no conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Hayden, M.J., Dixon, J.B., Dixon, M.E. et al. Characterization of the Improvement in Depressive Symptoms Following Bariatric Surgery. OBES SURG 21, 328–335 (2011). https://doi.org/10.1007/s11695-010-0215-y
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-010-0215-y