Abstract
Purpose
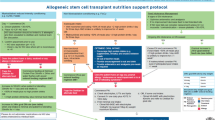
Effective, timely and evidence-based nutritional management is important in patients receiving autologous haematopoietic stem cell transplant (HSCT) to prevent the negative consequences of developing malnutrition. This study describes a robust process for development and implementation of an evidence-based nutrition care pathway for HSCT patients in a tertiary cancer centre.
Methods
A comprehensive review of the literature was completed to identify relevant articles and evidence-based guidelines to inform the development of the pathway. Evidence from the literature review was assessed and utilised to underpin the development of pathway. The pathway was implemented in the haematology service in collaboration with the multidisciplinary haematology team. Dietetic resource requirements for implementation of the pathway were determined and clinician compliance with the care pathway was assessed to evaluate the feasibility of the pathway in supporting delivery of evidence-based care.
Results
The evidence-based care pathway was implemented in 2011 with the final care pathway based on recommendations from five international evidence-based guidelines. Overall clinician compliance with delivering nutrition management described in the care pathway was high at 84%. The dietetic resource requirement for implementation of the care pathway was 300 to 400 h per 100 patients depending on conditioning chemotherapy regimen.
Conclusion
A robust process for developing and implementing a nutrition care pathway for HSCT patients was effective in supporting the delivery of evidence-based nutritional management for patients treated with HSCT.

Similar content being viewed by others
References
International Agency for Research on Cancer (IARC). GLOBOCAN 2012 v1.1 Cancer Incidence and Mortality Worldwide. IARC CancerBase No.11 2012 8th January 2018]; Available from: http://globocan.iarc.fr
Leukaemia Foundation. Leukaemia Foundation Homepage. [cited 2017 20th November]; Available from: http://www.leukaemia.org.au
Sonis ST, Oster G, Fuchs H, Bellm L, Bradford WZ, Edelsberg J, Hayden V, Eilers J, Epstein JB, LeVeque FG, Miller C, Peterson DE, Schubert MM, Spijkervet FKL, Horowitz M (2001) Oral Mucositis and the clinical and economic outcomes of hematopoietic stem-cell transplantation. J Clin Oncol 19(8):2201–2205
Wardley AM, Jayson GC, Swindell R, Morgenstern GR, Chang J, Bloor R, Fraser CJ, Scarffe JH (2000) Prospective evaluation of oral mucositis in patients receiving myeloablative conditioning regimens and haemopoietic progenitor rescue. Br J Haematol 110(2):292–299
Hébuterne X, Lemarié E, Michallet M, Beauvillain de Montreuil C, Schneider S, Goldwasser F (2014) Prevalence of malnutrition and current use of nutrition support in patients with Cancer. JPEN 38(2):196–204
Pressoir M, Desné S, Berchery D, Rossignol G, Poiree B, Meslier M, Traversier S, Vittot M, Simon M, Gekiere JP, Meuric J, Serot F, Falewee MN, Rodrigues I, Senesse P, Vasson MP, Chelle F, Maget B, Antoun S, Bachmann P (2010) Prevalence, risk factors and clinical implications of malnutrition in French Comprehensive Cancer Centres. Br J Cancer 102(6):966–971
Hung Y-C, Bauer J, Horsley P, Waterhouse M, Bashford J, Isenring E (2013) Changes in nutritional status, body composition, quality of life, and physical activity levels of cancer patients undergoing autologous peripheral blood stem cell transplantation. Support Care Cancer 21(6):1579–1586
Dickson TMC, Kusnierz-Glaz CR, Blume KG, Negrin RS, Hu WW, Shizuru JA, Johnston LL, Wong RM, Stockerl-Goldstein KE (1999) Impact of admission body weight and chemotherapy dose adjustment on the outcome of autologous bone marrow transplantation. Biol Blood Marrow Transplant 5(5):299–305
Horsley P, Bauer J, Gallagher B (2005) Poor nutritional status prior to peripheral blood stem cell transplantation is associated with increased length of hospital stay. Bone Marrow Transplant 35:1113–1116
Raynard B, Nitenberg G, Gory-Delabaere G, Bourhis JH, Bachmann P, Bensadoun RJ, Desport JC, Kere D, Schneider S, Senesse P, Bordigoni P, Dieu L (2003) Summary of the standards, options and recommendations for nutritional support in patients undergoing bone marrow transplantation. Br J Cancer 89(Suppl 1):S101–S106
Andersen S, Brown T, Kennedy G, Banks M (2015) Implementation of an evidenced based nutrition support pathway for haematopoietic progenitor cell transplant patients. Clin Nutr 34(3):536–540
Eccles MP, Mittman BS (2006) Welcome to Implementation Science. Implement Sci 1(1):1
Brown TE, Spurgin A-L, Ross L, Tripcony L, Keller J, Hughes BGM et al (2013) Validated swallowing and nutrition guidelines for patients with head and neck cancer: identification of high-risk patients for proactive gastrostomy. Head Neck 35(10):1385–1391
Hughes BGM, Jain VK, Brown T, Spurgin A-L, Hartnett G, Keller J, Tripcony L, Appleyard M, Hodge R (2013) Decreased hospital stay and significant cost savings after routine use of prophylactic gastrostomy for high-risk patients with head and neck cancer receiving chemoradiotherapy at a tertiary cancer institution. Head Neck 35(3):436–442
Kiss N, Krishnasamy M, Loeliger J, Granados A, Dutu G, Corry J (2012) A dietitian-led clinic for patients receiving (chemo)radiotherapy for head and neck cancer. Support Care Cancer 20(9):2111–2120
Odelli C, Burgess D, Bateman L, Hughes A, Ackland S, Gillies J, Collins CE (2005) Nutrition support improves patient outcomes, treatment tolerance and admission characteristics in oesophageal cancer. Clin Oncol 17(8):639–645
National Health and Medical Research Council (2009) NHMRC Levels of Evidence and Grades for Recommendations for Developers of Guidelines. Available from: http://www.nhmrc.gov.au/_files_nhmrc/file/guidelines/evidence_statement_form.pdf
Hakel-Smith N, Lewis NM (2004) A standardized nutrition care process and language are essential components of a conceptual model to guide and document nutrition care and patient outcomes. J Am Diet Assoc 104(12):1878–1884
Lacey K, Pritchett E (2003) Nutrition care process and model: ADA adopts road map to quality care and outcomes management. J Am Diet Assoc 103(8):1061–1072
Arends J, Bodoky G, Bozzetti F, Fearon K, Muscaritoli M, Selga G, van Bokhorst-de van der Schueren MAE, von Meyenfeldt M, Zürcher G, Fietkau R, Aulbert E, Frick B, Holm M, Kneba M, Mestrom HJ, Zander A (2006) ESPEN guidelines on enteral nutrition: non-surgical oncology. Clin Nutr 25(2):245–259
August DA, Huhmann MB (2009) A.S.P.E.N. Clinical guidelines: nutrition support therapy during adult anticancer treatment and in hematopoietic cell transplantation. JPEN 33(5):472–500
Bozzetti F, Arends J, Lundholm K, Micklewright A, Zurcher G, Muscaritoli M (2009) ESPEN guidelines on parenteral nutrition: non-surgical oncology. Clin Nutr 28(4):445–454
Isenring E, Zabel R, Bannister M, Brown T, Findlay M, Kiss N, Loeliger J, Johnstone C, Camilleri B, Davidson W, Hill J, Bauer J (2013) Updated evidence-based practice guidelines for the nutritional management of patients receiving radiation therapy and/or chemotherapy. Nutr Diet 70(4):312–324
Hagiwara S, Mori T, Tuchiya H, Sato S, Higa M, Watahiki M, Hoshina M, Mochizuki T, Chiba T, Miwa A, Kawachi S (2011) Multidisciplinary nutritional support for autologous hematopoietic stem cell transplantation: A cost–benefit analysis. Nutr 27(11):1112–1117
Hung YC, Bauer JD, Horsely P, Coll J, Bashford J, Isenring EA (2014) Telephone-delivered nutrition and exercise counselling after auto-SCT: a pilot, randomised controlled trial. Bone Marrow Transplant 49:786–792
Howard P, Jonkers-Schuitema C, Furniss L, Kyle U, Muehlebach S, Ödlund-Olin A, Page M, Wheatley C (2006) Managing the patient journey through enteral nutritional care. Clin Nutr 25(2):187–195
Kondrup J, Allison SP, Elia M, Vellas B, Plauth M (2003) ESPEN guidelines for nutrition screening 2002. Clin Nutr 22(4):415–421
Martin-Salces M, de Paz R, Canales MA, Mesejo A, Hernandez-Navarro F (2008) Nutritional recommendations in hematopoietic stem cell transplantation. Nutr 24(7):769–775
Botti S, Liptrott SJ, Gargiulo G, Orlando L (2015) Nutritional support in patients undergoing haematopoietic stem cell transplantation: a multicentre survey of the Gruppo Italiano Trapianto Midollo Osseo (GITMO) transplant programmes. ecancermedicalscience 9: 545
Muscaritoli M, Grieco G, Capria S, Paola Iori A, Rossi Fanelli F (2002) Nutritional and metabolic support in patients undergoing bone marrow transplantation. Am J Clin Nutr 75(2):183–190
Kiss N, Seymour J, Prince HM, Dutu G (2014) Challenges and outcomes of a randomised study of early nutrition support during autologous stem-cell transplation. Curr Oncol 2(12):e334–e339
Murray SM, Pindoria S (2009) Nutrition support for bone marrow transplant patients. Cochrane Database Syst Rev
Acknowledgements
The authors would like to thank the multidisciplinary haematology team for their support with the development and implementation of the care pathway. No funding was received to complete this work.
Author information
Authors and Affiliations
Contributions
All authors have made substantial contributions to the design of the study, collection or interpretation of data and writing the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
None to declare.
Rights and permissions
About this article
Cite this article
Atkins, L., Steer, B., Ray, H. et al. Implementing and sustaining an evidence-based nutrition service in a haematology unit for autologous stem cell transplant patients. Support Care Cancer 27, 951–958 (2019). https://doi.org/10.1007/s00520-018-4384-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00520-018-4384-x